The Ministry of Health needs your help to remember the principles of public health!
I argue that a recent consultation document pushes aside established principles of public health including proportionality, while framing discussion to promote a medicalised pandemic agenda.
Please, take the time to respond to this consultation. I’ve included the Ministry’s questions below - so before commencing to answer the questions, you might establish what the MoH’s scope of consultation is predominantly focussed on.
I’m not the only person dismayed by this draft paper, Guy Hatchard and The Looking Glass have commented as well.
The Ministry of Health needs your help to remember the principles of public health and basic public health norms. They seem to separate out a newly invented amalgam of ‘ethics’ that ignore long established public health ethics.
The established principles of public health are (a Google search should help):
Non-maleficence, Beneficence, Respect for autonomy, Proportionality, Health maximisation, Efficiency and Justice.
The Health Act 1956 provides a good foundation for discussion. The Act imposes an obligation on the Ministry of Health -
the Ministry shall have the function of improving, promoting, and protecting public health.
Part 3A Management of infectious diseases reflects many of the principles of public health - yet they were left out of all pandemic discussion by official actors.
The current discourse in this document appears to ignore these principles, reframe the definitions of ‘ethics’, and sweep the whole of the population into an ‘equity’-based intervention-led, compulsory vaccination surveillance and data state. This benefits both big pharma, big digital tech and big junk-food. Because it excludes the social, economic and political drivers of vulnerability to communicable and non-communicable disease it pushes out any political obligation to take firm steps to control big food and ensure our poorest and most vulnerable can access decent food.
Finally, it sets aside the fact that not all citizens are equally at risk, inferring that all of the population must hop on the ‘compulsory intervention bandwagon’ - or ladder (see image 5 below).
ETHICAL DELIBERATION OUT IN THE COLD 2019-2022
Despite these obligations in law, a bioethics panel was never-ever-ever convened. No meaningful ethics deliberation occurred, to balance and judge the evidence in the literature and the legislation that forced the inteventions on the general public. The obligations of the Health Act are not mentioned in the Ministry of Health document.
Why isn’t protection of health as a principle, enshrined at a high level in this NEAC document? Does this make it difficult to require governments to protect health - including judgement and discretion over interventions, and not just zero in on ‘infection’ or case risk, as I have oft discussed. Because what then happens is the resultant legislation becomes technocratic and unable to discern difference.
The 5 principles outlined in the July 2022 document: Tino rangatiratanga, equity, active protection, options, and partnership (p.8) predominantly focus on interventions as response measures.
They do not concern how we judge how health is stewarded and safeguarded.
It’s interesting that kaitiakitanga, which is associated with stewardship and protection, is not included. Public health traditionally is about protection and prevention - and proportionality.
Ethics is closely tied with how and what we value. So We don’t discuss ethics much, but we need to. Protection is a principle - it is a general and somewhat abstract. It intertwines with ethics, how and why do we draw attention and define danger, risk, what is right and wrong and how we take steps to prevent and protect individuals. Ethics tend to be closely associated with culture.
Of course the underpinning nuances can change - such as ethics being associated with general terms: Health and wellbeing, equity, Kotahitanga, Tika, Manaakitanga, Liberty. However what this does is persistently shift the narrative away from recognising that people are differently at risk. I have discussed this at length.
The soft tone ‘intervene’ instead of restrict - across the document - should be regarded cautiously. Because of the equity narrative - it means all should be treated with interventions equally. And of course, as we see in the ladder below, the interventions generally revolve around acceptance of a vaccine.
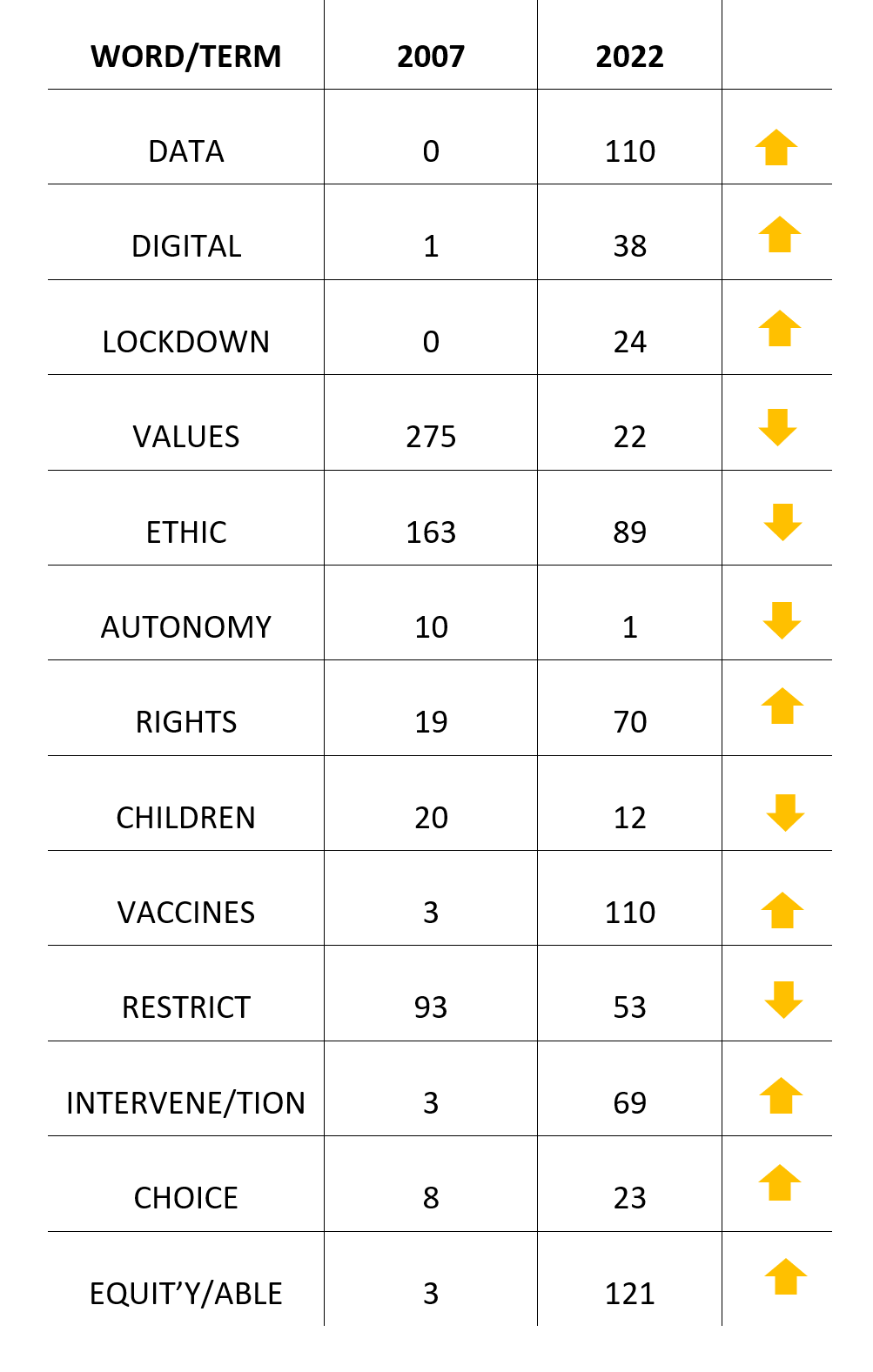
(Have a quick word count yourself to compare what the new MoH consultation focuses on, to understand how a massive shift has occurred since 2007. Word counts (Cntrl+F) are a simple tool to identify discourse & narrative shifts. This is a rough ‘back of the napkin’ count.)
It’s also evident that the references in the document disproportionately reflect the 2019-2022 pandemic experiences by governments, and the white and grey think tank literature often closely associated with governments and technology narratives.
This displaces, the last century of public health literature that focuses on the principles stated above.
The Ministry of Health (MoH) also apparently needs our help to remind them that immunisation was historically in place to prevent infection. New industry-friendly techniques to enforce vaccines that might prevent disease might not be proportionate nor ethical. All medicines carry risk. There seems to capacity for the MoH to look critically at the effect of global vaccination, conventional knowledge around herd immunity, and how interventions might be targetted, rather than globally applied.
PANDEMIC USED TO MEAN HIGH FATALITY.
We see that it is common now to conflate ‘pandemic’ with high risk event for an infectious disease that is not associated with high case fatality rates for the generally healthy. The Ministry of Health might not be aware that ‘pandemic’ situations today, are not necessarily associate with a high fatality rate across the population. This means that all ‘interventions’ are not equal as they can impose health harming and rights restricting interventions on not-at-risk people.
The WHO Pandemic Influenza Preparedness and Response 2009 document changed the definition of pandemic, changed the definition of severity, failed to discuss the role of natural immunity in achieving herd immunity, and introduced the prospect of global vaccination at scale.
Unlike the Spanish Influenza, COVID-19 did not carry the same severe mortality risk. Risk then was conflated around the spread of infection. This narrative effectively swept up the population into an infection-related fear-a-thon - because risk of hospitalisation and mortality was never based on risk by age or health status.
What has been excluded, is how we judge risk - this is closely tied to the principle of proportionality. Children, young people and healthy people who are not at risk of an infectious disease, should not have interventions forced apon them.
Why does the document not emphasise the protection of children’s and young people’s health? This is an important judgement, as medical and social interventions may have long term effects on children and young people’s health that do not impact adults. It is an important consideration (as the principle of proportionality) as children and young people may be less at risk of an infectious disease outbreak, but the government response may cause disproportionate harm. Therefore the government cannot be observed to protect health and prevent harm.
Why are vaccines and vaccination discussed only as a benefit, and why are interventions primarily based around vaccination?
What form of medicalisation is expected in the next ‘pandemic’ when we know that mRNA vaccine development has already gone into hyperdrive? What ‘choice’ will be given to the average healthy public?
PANDEMIC RISK - AGE & HEALTH STATUS
Risk in infectious disease pandemics are predicated on age and health status
The problem is, our hospitals are overwhelmed by patients with diet driven multimorbid conditions that are driven by access to cheap, addictive ultraprocessed food. Ultraprocessed foods damage metabolic health, and this is directly associated with immune status and mental health status.
Risks from diet driven chronic disease, and the associated risk of obesity, were well known from the commencement of the pandemic. Yet the government rarely articulated this risk and did not take measures to ameliorate this risk.
I’ve discussed at length, the fact that all the politically-appropriate discussion on medical equity in the world. cannot address the drivers of multimorbidity. The cost of multimorbidity is super-additive. Multimorbidity drives risk to infectious disease as well as mental illness.
Because it’s political, it would involve taxing junk food and rediverting the proceeds to wholefoods. (If we can do all the smart algorithms and data modelling, why can’t societies do this?)
What actions are taken in policy to reduce the drivers of metabolic disease and obesity across populations in order to improve health for the groups most at risk?
As we see again and again in these documents, the drivers of disease are left out of policy, and medical equity is conflated as health equity. Sir Micheal Marmot has identified this as a key issue for decades.
To make a fundamental improvement in health equity, technical and medical solutions such as disease control and medical care are, without doubt, necessary. But they are insufficient.
New Zealand’s food environment is obesogenic. The voice of nutrition in New Zealand is alarmingly quiet.
Somehow the wellbeing government can’t address inequality, and can’t tax addictive ultraprocessed food, and ignores the fact that foodbanks, despite their best (bootom of the cliff) efforts, offer low nutrient ultraprocessed food that cannot promote health.
Why can’t our government address the drivers of risk in a pandemic via a suite of measures?
REPURPOSING AN INTERVENTION LADDER TO PROMOTE VACCINES
Why would vaccines be considered mandatory for not at risk people?
We can see that the MoH repurposed the Nuffield ‘Intervention Ladder’ to pop the word ‘vaccine’ through it. This demonstrates that vaccines are considered the most critical intervention, and sets aside more nuanced discussion relating to who is at risk.

(And of course, as if to anticipate such policy, a veritable plethora of mRNA gene therapy vaccines are in development.)
Finally, while theoretically the NEAC is independent, this does not appear to be the case in 2022. In 2007 the committee and secretariat were noted. In 2022 the Ethical Guidance for a Pandemic is simply branded NEAC and MoH. There’s no indication anyone paid outside direct MoH has input. There’s no indication experts with a strong public health background who are versed in the principles of public health have partipated.
End JRBruning comments.
The consultation is available here:
https://consult.health.govt.nz/ethics/egap/
Ministry of Health Consultation. Closes 20 Sep 2022
The National Ethics Advisory Committee – Kāhui Matatika o te Motu (NEAC) is an independent advisor to the Minister of Health. NEAC has developed an update to its 2007 publication ‘Getting Through Together: Ethical Principles for a Pandemic’. The updated publication is called ‘Ethical Guidance for a Pandemic: Whakapuāwaitia e tatou kia puāwai tātoui’. This online survey is seeking your feedback on the draft publication.
NEAC wants to know if the ideas contained within the publication are shared ideas based on shared values. Contributions from all voices, individuals, communities and organisations are welcomed and encouraged. This consultation provides an opportunity to inform the ethical guidance for future pandemics in Aotearoa New Zealand, as well as the ongoing Covid-19 pandemic. You can submit on your own behalf or on behalf of an organisation. Your submissions will be taken into consideration by NEAC and may be used to make improvements to the draft publication before it is published.
Question 1a. Which of the proposed seven foundational elements to Aoteaora New Zealand’s pandemic response do you agree with? (tick as many as apply)
Honouring Te Tiriti o Waitangi
Developing a strong and well-functioning health system
Building back better – getting ready for the future
Adopting Te Whare Tapa Whā – a shared model of health and wellbeing
Embedding mātauranga Māori
Taking an intersectional approach
Upholding human rights
Question 1b. If you have any comments about the seven foundational elements, please explain below. Are there any foundational elements you want added, removed, or significantly changed? If you have no comments, you may leave this blank.
Chapter two sets out six ethical principles (pages 12-17) for Aotearoa New Zealand to apply during a pandemic. These are designed to be shared principles that offer a shared basis for decision-making. The principles are interconnected and relate strongly to each other.
The six principles are:
Health and wellbeing (page 14)
Equity (page 14)
Kotahitanga (page 15
Manaakitanga (page 15-16)
Tika (page 15)
Liberty (page 17).
Question 2a. Which of the six ethical principles proposed for Aotearoa New Zealand to apply during a pandemic do you agree with? (tick as many as apply)
· Health and wellbeing Kotahitanga Tika Equity Manaakitanga Liberty
Question 2b. If you have any comments about the six ethical principles, please add them below. Are there any ethical principles you want added, removed, or significantly changed? If you have no comments, you may leave this blank.
Chapter two also outlines a framework (page 18) for making ethically complex public health decisions in a pandemic. Public health focuses on groups of people rather than individuals and could involve decisions about a wide range of situations or services that impact the Te Whare Tapa Whā (pages 9-10) model of health. The seven elements of the framework are identified as:
Transparency
Consistency
Justification
Participation
Managing conflicts of interest
Openness for revision
Regulation.
Question 3a. Do you agree that these elements combine to create a useful process for decision-makers to use in a pandemic?
Strongly disagree
Disagree
Neutral
Agree
Strongly agree
Select your answer
Question 3b. If you have any comments about these elements, please add them below. Do you have any other suggestions about how we can ethically make complex public health decisions? If you do not have any comments, you may leave this blank.
Chapter three outlines the ethical importance of Aotearoa New Zealand being ready for the next pandemic (pages 19-27), emphasising:
Preparing our health and disability system (pages 21-22)
Health investment (pages 22-24)
Digital inclusion (page 24); and
Community readiness (pages 25-27).
Question 4. If you have any comments about the section on preparing our health and disability system, please leave them below. Is there information you want added, removed, or substantially changed in this section? If you do not have any comments, you may leave this blank.
Question 5. If you have any comments about the section on health investment, please leave them below. Is there information you want added, removed, or substantially changed in this section? If you do not have any comments, you may leave this blank.
Question 6. If you have any comments about the section on digital inclusion, please leave them below. Is there information you want added, removed, or substantially changed in this section? If you do not have any comments, you may leave this blank.
Question 7. If you have any comments about the section on community readiness, please leave them below. Is there information you want added, removed, or substantially changed in this section? If you do not have any comments, you may leave this blank.
Chapter three also outlines ‘reduction of risk’ (pages 28-29) or steps that Aotearoa New Zealand can take to reduce the likelihood of a pandemic beginning here or overseas. This section emphasises environmental risks and global cooperation.
Question 8. If you have any comments about the section on reduction of risk, please add them below. Is there information you want added, removed, or significantly changed? For example, are there any other risk reduction factors that should be taken into account? If you do not have any comments, you may leave this blank.
Chapter four outlines ethical issues in responding to a pandemic. This chapter includes an ethical review of: interventions to improve a pandemic situation (pages 30-36)
Question 9. The section on justification for interventions (pages 30-31) outlines that interventions designed to slow or eliminate the spread of a pandemic should align with the national ethical principles, and they must reflect four further considerations. Do you agree with these considerations (stated below)?
Strongly disagree
Disagree
Neutral
Agree
Strongly agree
a. When possible and appropriate, restrictions should be agreed rather than imposed.
b. Imposed restrictive measures should aim to minimise any limitation of human rights and carefully describe the justification for that limitation. Special attention may be needed for people who are subject to restrictions (for example, to their freedom of movement) to ensure their other rights are protected.
c. Reciprocal support may be appropriate for people who, to protect others, have restrictions imposed upon them.
d. Restrictive measures can be justified only when all the narrowly defined circumstances set out in human rights law, known as the Siracusa Principles (page 31), are met.
Question 10. How appropriate are the Siracusa Principles (page 31), for Aotearoa? Are there other more appropriate principles that could guide intervention? If you do not have any comments, you may leave this blank.
Chapter four outlines ethical issues in responding to a pandemic. This chapter includes an ethical review of: interventions to improve a pandemic situation (pages 30-36)
Question 11a. The section on justification for restricting choice (pages 32-33) discusses examples where restricting or removing choice in a pandemic might be justified. Which of these examples do you agree with? Tick all that apply.
Ensuring the intervention is widely utilised and its benefits obtained Preventing the need for more restrictive measures later Protecting those who are more at risk of being affected by the pandemic due to pre-existing inequities
Question 11b. If you have any comments on these examples, please add them below. Are there other examples that you think we should discuss? If you do not have any comments, you may leave this blank.
Question 12. If you have any comments about the section on effects of interventions (pages 34-36), please add them below. Are there any other effects of interventions that we haven’t listed that are likely to be relevant in future pandemics? If you do not have any comments, you may leave this blank.
Chapter four outlines ethical issues in responding to a pandemic. This chapter also includes an ethical review of:
communications and engagement during a pandemic (pages 37-39)
data, privacy, and digital technologies in a pandemic (pages 39-44).
Question 13. If you have any comments on the communications and engagement section (pages 37-39), please add them below. Is there information you want added, removed, or substantially changed in this section? If you do not have any comments, you may leave this blank.
Question 14. If you have any comments on the data, privacy and digital technologies section (pages 39-44), please add them below. Is there information you want added, removed, or substantially changed in this section? If you do not have any comments, you may leave this blank.
Chapter five outlines the path of recovery (pages 45-50), emphasising relevant ethical considerations, including:
vaccine development and use (pages 45-48)
Question 15. The section on vaccine development and use (pages 45-48) considers many ethical issues. How much do you agree with these ethical statements?
Strongly disagree
Disagree
Neutral
Agree
Strongly agree
a. Priority access to vaccines should be given to the most vulnerable people in a pandemic (Equity, page 46).
b. Ideally, vaccination should be voluntary rather than non-voluntary (Levels of coerciveness, page 46).
c. The use of vaccine certificates must be based on scientific evidence that they are effective at achieving their stated outcome (e.g. preventing spread of the pandemic) (Vaccine Certificates – Efficacy, pages 46-47).
d. If a vaccine certificate is required to access essential goods and services, vaccines are no longer truly voluntary. (Vaccine Certificates – Supplementary effects, page 47).
e. People who cannot safely receive the vaccine for medical reasons should be given an exemption to vaccine certificate requirements (Vaccine Certificates – Equity, page 47).
f. Global cooperation is required to ensure fair and equitable access to vaccines in low-to-middle-income countries (Global cooperation, page 48).
Chapter five outlines the path of recovery (pages 45-50), emphasising relevant ethical considerations. This also includes:
reopening (pages 48-49), and
ongoing impacts (page 50)
Question 16. If you have any comments on the section on reopening, please leave them below. Is there information you want added, removed or substantially changed in this section? If you do not have any comments, you may leave this blank.
Question 17. If you have any comments on the section on ongoing impacts, please add them below. Is there information you want added, removed or substantially changed in this section? If you do not have any comments, you may leave this blank.
Chapter six (pages 51-58) focuses solely on the ethical considerations of and for disabled people in a pandemic. The Chapter is similarly structured to reflect ‘readiness and reduction of risk’, ‘response’, and ‘recovery’.
Question 18a. How well does the section on readiness and reduction of risk (pages 52-55) capture the relevant ethical issues for disabled people?
Very poorly
Poor
Neutral
Well
Very well
Select your rating
Question 18b. If you have any comments on this section, please add them below. Is there information you want added, removed or substantially changed in this section? If you do not have any comments, you may leave this blank.
Question 19a. How well does the section on response (pages 55-57) capture the relevant ethical issues for disabled people?
Very poorly
Poor
Neutral
Well
Very well
Select your rating
Question 19b. If you have any comments on this section, please add them below. Is there information you want added, removed or substantially changed in this section? If you do not have any comments, you may leave this blank.
Question 20b. If you have any comments on this section, please add them below. Is there information you want added, removed or substantially changed in this section? If you do not have any comments, you may leave this blank.
Overarching questions
Question 21. If you have any comments on the structure of the publication, please leave them below. If you do not have any comments, you may leave this blank.
Question 22. If you have any further comments on the publication, please add them below. If you do not have any comments, you may leave this blank.
Your information
The following optional questions are asked in order to understand how different communities in Aotearoa New Zealand respond to this document. The demographic data is collected to assist in the analysis of results. If you choose to provide contact information, this may also be used to request follow up information about your submission.
If you are completing this survey on your own behalf, please answer questions B to H below after answering question A.
If you are completing this survey on behalf of an organisation, please skip to question I below after answering question A.
Further questions